
The Neuropsychiatry of Tinnitus: A Circuit-Based Approach to the Causes and Treatments Available
Mia T Minen, Joan Camprodon, Romy Nehme, Zeina Chemali | J Neurol Neurosurg Psychiatry. 2014;85(10):1138-1144.
Copyright © 2014 by WebMD LLC. All rights reserved.
Abstract and Introduction
Abstract
Patients presenting with tinnitus commonly have neuropsychiatric symptoms with which physicians need to be familiar. We provide an overview of tinnitus, including its types and pathophysiology. We discuss how recent methods such as transcranial magnetic stimulation, positron emission tomography, MRI, magnetoencephalography and quantitative EEG improve our understanding of the pathophysiology of tinnitus and connect tinnitus to the neuropsychiatric symptoms. We then explain why treatment of the tinnitus patient falls within the purview of neuropsychiatry. Psychiatric problems such as depression, anxiety and personality disorders are discussed. We also discuss how stress, headache, cognitive processing speed and sleep disturbance are associated with tinnitus. Finally, we provide a brief overview of treatment options and discuss the efficacy of various medications, including benzodiazepines, antidepressants, antipsychotics and mood-stabilising agents, and various non-pharmacological treatment options, such as cognitive behavioural therapy, habituation therapy and acupuncture. We also discuss how brain stimulation therapies are being developed for the treatment of tinnitus. In conclusion, a review of the literature demonstrates the varied neuropsychiatric manifestations of tinnitus. Imaging studies help to explain the mechanism of the association. However, more research is needed to elucidate the neurocircuitry underlying the association.
Introduction
Chronic tinnitus, or the perception of sounds without an external source, afflicts 10–15% of the population.[1] The sounds may be described as ringing, roaring, hissing or pulsatile, to name a few adjectives.[2,3] Traditional classification systems describe two forms of tinnitus: objective and subjective. Objective tinnitus is less common and consists of a sound that can be heard by both the patient and the physician. Examples of objective types include arterial bruits, venous hums, palatal myoclonus and stapedial myoclonus. The subjective form is only appreciated by the patient.[2,4]
Tinnitus occurs commonly with certain forms of peripheral or central abnormality. There are cochlear pathologies associated with hearing loss and tinnitus—for example, noise-induced damage, Meniere’s or acoustic neuroma.[2,5,6] Interestingly, in the case of acoustic neuroma, the incidence and duration of tinnitus is increased in patients with the smallest tumours.[7] Autoimmune disorders such as diabetes can cause vestibular nerve dysfunction.[8] Tinnitus can also have central causes such as stroke, demyelinating lesions and arteriovenous malformations.[2,5,6] Tinnitus may be caused by trauma, as further described below, and it may be both triggered by and treated with antidepressants.
Early formulations of tinnitus explained this condition strictly as a disorder of the auditory system, the neurophysiological model of Jastreboff being a notable exception.[9] As evident from the epidemiological and clinical data we provide, it is the norm and not the exception that patients with tinnitus present with cognitive, behavioural and affective symptoms. We propose that these non-auditory symptoms are not just comorbidities, but core components of the tinnitus syndrome, which is neuropsychiatric in nature (figure 1). Interestingly, the perceptual characteristics of tinnitus (frequency, loudness) do not appear to be correlated with other symptoms, life satisfaction, sleep or handicap from the tinnitus.[10]
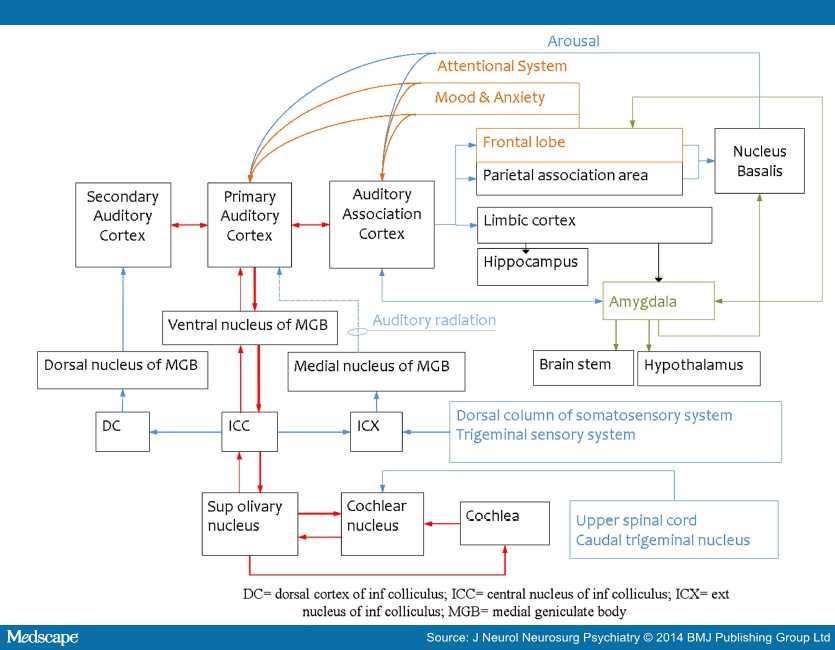
Following a discussion about the associated symptoms of tinnitus and a brief overview of treatment options, we show how recent imaging studies connect tinnitus to the neuropsychiatric comorbidities and suggest possible brain circuitry systems for this association.
